Differentiating Pudendal Nerve Entrapment (PNE) from Other Pelvic Conditions
Diagnosing pudendal nerve entrapment can be challenging because its symptoms often mimic those of other pelvic disorders, such as:
- Piriformis syndrome
- Interstitial cystitis
- Vulvodynia
- Prostatitis
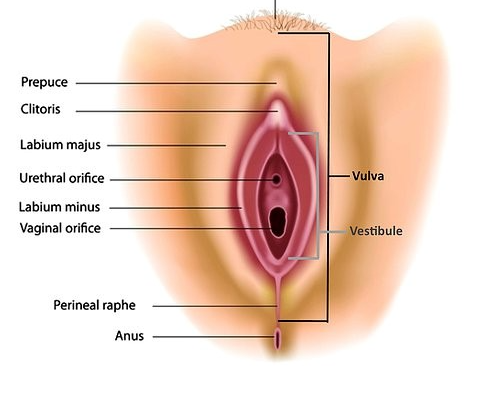
Vulvodynia is a chronic pain condition affecting the vulvar area in women, known for its potential to substantially impact the quality of life. This condition is characterized by persistent, unexplained pain in the vulva, the external female genitalia. Despite its prevalence, it remains a poorly understood condition. In this blog post, we delve into what vulvodynia is, explore treatment options, discuss vulvodynia bands, and examine the different self-care strategies that can help manage symptoms more effectively.
Vulvodynia
Vulvodynia is characterized by chronic vulvar pain or discomfort, with symptoms such as burning, stinging, irritation, or rawness. The pain can be localized to one area of the vulva or be more generalized, affecting various parts. The exact cause of vulvodynia is still unknown, but it’s thought to result from a combination of genetic, biological, and environmental factors. The condition can last for several months to years and can significantly impair sexual function, psychological well-being, and quality of life.
Vulvodynia Treatment
Managing vulvodynia typically involves a multidisciplinary approach aimed at reducing pain and improving function.
- Medications:
– Antidepressants, anticonvulsants, and topical anesthetics can help manage the pain associated with vulvodynia.
– Estrogen creams may also be prescribed to alleviate symptoms in some cases.
- Physical Therapy:
– Pelvic floor physical therapy can assist in reducing muscle tension and pain in the pelvic floor muscles.
- Cognitive-Behavioral Therapy (CBT):
– CBT can be beneficial in addressing the emotional stress and psychological impact associated with chronic pain conditions like vulvodynia.
- Biofeedback and Neurostimulation:
– These can be helpful in modulating the pain perception and improving the overall quality of life for women with vulvodynia.
- Surgical Intervention:
– In severe, localized cases of vulvodynia, vestibulectomy, a surgical removal of the affected tissue, may be considered.
Vulvodynia Band
A vulvodynia band is a specially designed support garment to alleviate the discomfort associated with vulvodynia. It usually provides gentle compression, helping to reduce pain and inflammation in the vulvar area.
- Functionality:
– The band can aid in reducing pressure and friction in the affected area, especially during physical activities, providing relief from symptoms.
- Use:
– It can be particularly useful for those who experience pain while sitting or engaging in activities, offering support and cushioning to the vulvar area.
- Availability:
– These bands are usually available online or through specialized providers, offering a non-invasive, practical solution for daily symptom management.
Vulvodynia Self-Care
Managing vulvodynia effectively also involves adopting various self-care strategies.
- Avoid Irritants:
– Use unscented, mild soaps and avoid potential irritants like dyes and fragrances in clothing and laundry detergents.
- Wear Cotton Underwear:
– Opt for loose, breathable cotton underwear and avoid tight-fitting clothes to reduce irritation.
- Use Lubricants:
– Water-soluble lubricants can minimize discomfort during sexual intercourse.
- Manage Stress:
– Regular exercise, relaxation techniques, and stress management can play a crucial role in managing symptoms.
Vulvodynia is a challenging and often frustrating condition due to its chronic nature and the lack of a definitive cure. However, a combination of medical treatments, the use of vulvodynia bands, and appropriate self-care measures can significantly help manage the symptoms and improve the quality of life for those affected. Although the journey with vulvodynia can be daunting, comprehensive care, support, and informed management strategies can make it more navigable and bearable.